When degenerative changes, injuries, deformity, or tumors threaten the stability of the spinal column, spinal fusion can become a crucial procedure. The spine includes three main regions—cervical, thoracic, and lumbar—and when any region becomes unstable, the bony elements may compress delicate nerve tissue, putting the spinal cord and nerve roots at risk.
At Princeton Neurological Surgery, spinal fusion procedures are performed by a neurosurgical team led by board-certified neurosurgeon Dr. Edward H. Scheid, Jr. With more than 6,000 spine surgeries performed, Dr. Scheid is known for a careful, step-by-step approach to diagnosis and treatment planning—only recommending surgery when it is clinically indicated and tailoring care to each patient’s condition.
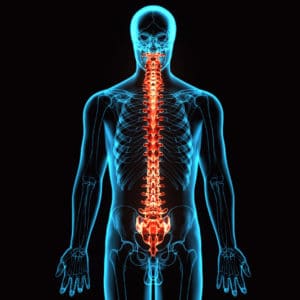
Why Spinal Fusion Can Be So Important
The main concern of an unstable spine is the tendency for the bony elements to compress delicate neural tissue. While an intact vertebrael column protects structures such as the spinal cord and nerve roots, an unstable vertebrael column threatens irreversible neurologic damage. In certain cases—especially when the cervical spine is involved—ongoing compression may contribute to progressive neurologic dysfunction, including weakness, loss of bodily function, and even paralysis. When spinal fusion is clinically indicated, it can help preserve neurologic function and restore structural stability.
What Are The Goals Of Spinal Fusion Surgery?
The two main goals of spinal fusion are:
- To decompress and preserve the function of the spinal cord and nerve roots
- To restore the structural integrity of the spinal column
Compression of the spinal cord and nerve roots may occur from a degenerative spinal column, a compressing tumor, or other injuries. Chronic degenerative changes affect the cervical and lumbar spinal column more often than the thoracic segment. The spinal column may become unstable prior to surgery or may become unstable after the neural elements have been decompressed during surgery. In other words, sometimes it is necessary to destabilize the spinal column in an effort to adequately free the nervous tissue from bony compression during spinal surgery. Therefore, spinal fusion candidates may not necessarily have unstable spinal columns prior to surgery.
Common Reasons Spinal Fusion May Be Recommended
These are some typical reasons a spine surgeon could recommend fusion surgery:
- Broken Vertebrae: Not all broken or cracked vertebraee require fusion, as some can heal. But if a fracture is creating instability, fusion may be necessary.
- Herniated Disc: When a disc herniates and needs to be removed, fusion may be necessary to stabilize the spine.
- Spinal Weakness Or Instability: With osteoporosis or osteoarthritis, excessive motion can occur between vertebraee. Fusion eliminates this abnormal motion.
- Spondylolisthesis: One vertebrae slips forward onto the vertebrae below it. If this causes nerve compression with numbness or weakness, fusion may be necessary.
- Spinal Deformities: Fusion can help correct scoliosis (curvature) or kyphosis (abnormal rounding of the upper spine).
Who Should Consider Spinal Fusion Surgery?
Spinal fusion may be appropriate for patients:
- Who have suffered trauma to the spinal column
- With spondylolisthesis or spondylosis
- With large disc herniations causing spinal cord compression (especially in the cervical or thoracic spinal column)
- With significant spinal canal stenosis that may require destabilizing decompressive surgery
Qualified surgeons are responsible for identifying patients who are appropriate candidates for spinal fusion and must decide whether it should be performed urgently. Sustained compression of the neural elements can result in permanent neurologic dysfunction and lead to numbness, weakness, loss of bodily functions and/or paralysis. Therefore, it may be a serious mistake to avoid or delay spinal fusion in certain cases. Although failed fusions can occur, they are much less likely in the hands of an experienced and well-trained spinal surgeon.
How Spinal Fusion Is Performed
The patient is under general anesthesia for this surgery. Regardless of the method, this is the usual process:
- Making The Incision: To gain access to the vertebraee, an incision may be made in the neck or back directly over the spine (posterior), on either side of the spine, or in the abdomen or throat (anterior). Necessary muscle and tissue are moved to access the spine.
- Disc Removal And Graft Placement: The disc is removed between the two vertebraee to be fused. Often this disc has herniated and is pushing on the adjacent spinal cord or nerve roots. Bone graft material replaces the disc. The graft may come from a bone bank, the patient’s body (often the pelvis), or synthetic material.
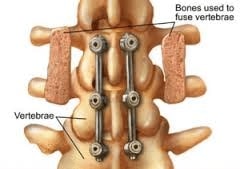
- Fusion And Stabilization: Bone graft material fuses the vertebraee together permanently. To keep the vertebraee stable while the graft grows, the vertebraee may be secured with a plate and screws or with vertical rods and screws, depending on location and need.
What Recovery Time Should I Expect After Spinal Fusion?
After spinal fusion surgery, patients are usually in the hospital for two to three days. Pain and discomfort are expected and are managed with medication. Spinal X-rays are typically obtained before discharge. Stitches are often removed in about 10 days, and follow-up visits commonly occur around 4–6 weeks, 6 months, one year, and two years.
Recovery takes commitment. It can take six months to a year for the spine to fully heal. Physical therapy is often important and ongoing. For the early healing period, patients are typically advised to avoid twisting, bending, and heavy lifting (often anything heavier than a gallon of milk), based on individualized guidance.
Risks Of Spinal Fusion Surgery
Spinal fusion is generally safe, but it includes the usual surgical risks such as infection, poor wound healing, excessive bleeding, blood clots, and nerve damage.
Beyond the immediate risks, fusing vertebraee changes how the spine handles loads. Because two vertebraee become one, stress can shift to adjacent segments. This added stress may accelerate wear and tear in the joints above or below the fusion over time.
Why Choose Princeton Neurological Surgery For Spinal Fusion?
Princeton Neurological Surgery is led by board-certified neurosurgeon Dr. Edward H. Scheid, Jr., who has performed more than 6,000 spine surgeries and is known for a precise, step-by-step approach to identifying the true cause of symptoms. Our team emphasizes careful diagnosis, detailed imaging review, and individualized treatment planning—recommending fusion only when it is clinically necessary to protect neurologic function and restore stability. With experience across complex spine conditions and advanced surgical techniques, we focus on outcomes that improve mobility, reduce pain, and help patients return to daily life with greater confidence.
Schedule A Spinal Fusion Consultation In Hamilton, NJ
Princeton Neurological Surgery has offices in Hamilton, NJ and serves patients from Hamilton and Jersey City—call (609) 890-3400 to schedule a consultation.