Chronic low back pain is a modern epidemic that carries a significant socioeconomic impact. The incidence of disability due to back pain has risen faster than that associated with any other medical condition and is the second-most frequent reason for patients to seek medical care. Although most episodes of back pain eventually resolve, a significant number of individuals continue to suffer chronic pain and disability.
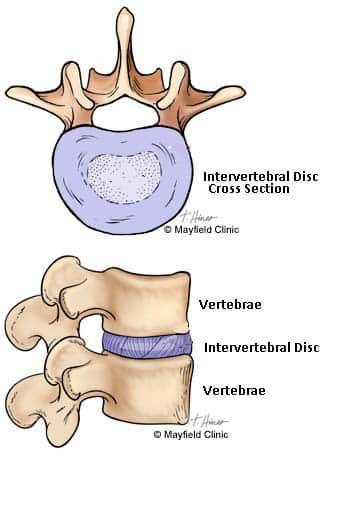
The spinal column is comprised of interlocking vertebrae separated by intervertebral discs. It provides load-bearing support for one-half of the body’s mass and protects the neural elements. The intervertebral discs provide shock absorption and facilitate the bending of the spine. The combination of the vertebrae and discs at each vertebral segment allow for motion of the spine including flexion, rotation, and extension. The motion and support functions of the spine in combination with the many interlocking vertebrae, nerves, and muscles, can result in back pain attributable to multiple causes.
What is Discogenic Back Pain?
Discogenic back pain is a chronic debilitating disorder originating from within the intervertebral disc. Pain fibers are thought to be recruited to the site of injury or degeneration within the disc. Therefore degenerative disc disease AKA, DDD as well as disc herniation or disc rupture can result in discogenic back pain.
Diagnosis of Discogenic Back Pain
Diagnosis of discogenic back pain can be difficult. There are characteristic findings on physical examination, but similar findings are seen in patients with other types of back pain as well. Imaging studies can also be performed such as MRI that may reveal the characteristic black disc. However, because disc degeneration is part of the normal aging process, MRIs often reveal abnormalities in patients with no symptoms. Therefore, it is difficult to ensure that disc pain is truly causing the symptoms, even if the disc appears abnormal on MRI.
A common test used to diagnose discogenic back pain is discography. During discography or discogram, a needle is placed into the center of the affected disc and a small amount of contrast dye is injected.
A CT scan and fluoroscopy (real-time x-ray) are used to visualize the morphology and integrity of the disc while provocative testing helps to identify the source of pain. Provocative testing is performed by increasing the pressure within the disc. The increased pressure simulates the patient’s back pain provided the disc being tested is the culprit.
The combination of abnormal morphology and concordant pain during provocative testing is generally considered a positive test for discogenic back pain. Diagnostic discography is used most often in conjunction with clinical evaluation by neurosurgeons prior to performing lumbar fusion in an effort to help support the location of the patient’s pain generator.
What People Say About Us!
"Dr. Lipani and his staff are excellent. Dr. Lipani was very thorough. He explained what needed to be treated and why. He has terrific bedside manners. He answered all my questions patiently. Did not rush me at any time. I recommended him to one of my friends and she was extremely happy with him too."
Click here to read more reviews.
Treatment and Surgery for Discogenic Back Pain
Several therapies have been used to target the painful nerve endings within the affected discs in patients with discogenic back pain. Non-surgical techniques include applying heat to the affected area, physical therapy, medication, and trans-dermal electrical nerve stimulation. However, non-surgical treatments are often ineffective in treating chronic back pain long-term.
There are a number of minimally invasive surgical procedures that are used to treat discogenic back pain, all of which have varying degrees of success. Intradiscal electrothermal therapy (IDET), involves the application of heat directly to the inside of the disc using a needle that is inserted under x-ray guidance. The goal of this technique is to destroy the offending nerves within the affected disc. This technique has varying degrees of success and pain relief is generally temporary. The problem with IDET and similar minimally invasive techniques is that destruction of pain fibers within the disc is variable and incomplete.
Spinal cord stimulation is another minimally invasive method used for treating discogenic back pain. This can be performed using a transcutaneous approach but sometimes requires an open approach that exposes a portion of the lower thoracic spinal cord for placement of electrodes. The electrodes are used to interfere with spinal cord pain signals to the brain. However, despite its minimally invasive potential, this technique has many drawbacks and therefore is generally reserved for when all other methods including open surgery, have failed.
Other conventional surgical approaches are used when other less invasive therapies are unsuccessful. The goal of surgery for discogenic back pain is to remove the offending disc and replace it with a bone plug. This technique involves fusing the adjacent vertebral bodies together so that there is no longer any motion between them. The bone plug that replaces the disc is what fuses to the vertebral bodies above and below the plug. This technique requires placement of internal hardware to secure the spinal column while the fusion process takes place. The loss of motion is negligible with respect to patient mobility and virtually all patients do not notice any restrictions. Alternatively, a titanium artificial disc may be used in place of the bone plug. This method preserves motion between the vertebrae and may be chosen to prevent adjacent discs from further degeneration in select cases. The recovery time varies from 3-4 months with these techniques.
At Princeton Neurological Surgery, Dr. Lipani is a board certified fellowship trained spine surgeon in New Jersey who performs minimally invasive spine surgery as well as complex spinal procedures. Dr. Lipani is a specialist in the treatment for discogenic back pain and many other spinal conditions such as spinal stenosis, herniated discs, degenerative disc disease, low back pain, neck pain, spinal tumors, spinal cancer and more. Dr. Lipani treats patients from around the world, New York, Pennsylvania, and New Jersey including locally from Princeton, New Brunswick, Hopewell, Pennington and communities throughout Somerset, Middlesex, Ocean, Burlington, Monmouth, Morris and Mercer Counties for discogenic back pain. Dr. Lipani offers image guided spine surgery approaches for discogenic back pain treatment, tailored to the needs of each patient.
At Princeton Neurological Surgery, careful patient selection and strategic operative planning ensures excellent outcomes. If you’ve been diagnosed with discogenic back pain and have failed conservative therapies, you may be a candidate for surgical intervention. Feel free to contact us about how we can help restore your quality of life and get feet on your back again!
Dr. Lipani’s affiliation with several major New Jersey hospitals means that you will receive degenerative disc disease surgery you need without having to travel to New York or Philadelphia. Dr. Lipani has over 15 years of experience performing brain and spine surgeries, so you can count on him to provide the best possible quality of care to all his patients.