Traditionally, spine surgery has been performed using open techniques that require longer incisions to allow direct visualization of the spine. While effective, open surgery often involves greater muscle disruption and longer recovery. Advances in technology and surgical technique now allow many spinal conditions to be treated using minimally invasive approaches.
At Princeton Neurological Surgery, minimally invasive spine surgery is performed by a neurosurgical team led by board-certified neurosurgeon Dr. Edward H. Scheid, Jr., who has performed more than 6,000 spine surgeries. Patients in Hamilton and Jersey City, NJ benefit from carefully selected minimally invasive techniques designed to reduce tissue disruption while maintaining surgical precision and safety.
What Is Minimally Invasive Spine Surgery?
Minimally invasive spine surgery (MISS) allows surgeons to access deep spinal structures through small incisions using specialized instruments and real-time fluoroscopic (x-ray) image guidance. These techniques minimize soft tissue disruption, reduce blood loss, and often result in faster recovery compared to conventional open surgery.
Smaller incisions typically mean:
- Less muscle manipulation
- Reduced postoperative pain
- Shorter hospital stays
- Quicker return to daily activities
Many minimally invasive procedures can be performed on an outpatient basis.
However, not all spinal conditions are appropriate for minimally invasive techniques. In some cases, direct visualization of delicate neural or vascular structures is necessary. Proper patient selection is critical to maintaining safety and achieving optimal results.
When Spine Surgery Becomes Necessary
Spine surgery is generally recommended after nonsurgical treatments fail to relieve symptoms. Conservative care may include:
- Pain medication
- Physical therapy
- Epidural steroid injections
- Chiropractic care
- Activity modification
Urgent surgical intervention may be necessary when symptoms such as acute weakness, loss of sensation, or bowel and bladder dysfunction develop. Careful evaluation determines whether surgery is immediately required or whether conservative therapy should continue.
Open Spine Surgery Vs. Minimally Invasive Techniques
In traditional open spine surgery, a midline incision is made and muscles are retracted to expose the vertebraee. Bone removal, decompression, and fusion instrumentation are performed through direct access.
In minimally invasive procedures, small incisions are made slightly off midline. Tubular retractors are inserted to create a narrow channel to the spine. These retractors gently separate muscle fibers rather than cutting them. Specialized elongated instruments are passed through the tubular system to remove disc or bone material and place screws or rods if needed.
Fluoroscopy provides real-time imaging throughout the procedure, and in some cases an operating microscope enhances visualization. When the procedure is complete, the retractor is removed and muscles return to their natural position, limiting tissue damage.
Common Minimally Invasive Spine Procedures
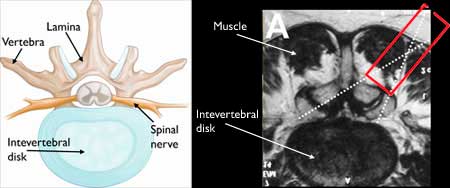
Minimally invasive techniques can be used for several spinal procedures, including:
- Lumbar discectomy
- Decompression procedures such as laminectomy
- Spinal fusion, including minimally invasive TLIF
Common Minimally Invasive Spine Procedures
MIS Lumbar Discectomy
For herniated discs compressing nerves, a small incision is made over the affected level. A retractor is inserted, and a small portion of bone may be removed to access the disc. The compressed nerve is gently retracted, and the herniated disc material is removed.
MIS Lumbar Fusion
In minimally invasive fusion procedures, such as TLIF, retractors are placed on either side of the spine to preserve midline structures. The disc is removed, bone graft is placed, and screws or rods are inserted through small incisions to stabilize the spine.
Anesthesia During MIS Procedures
Most minimally invasive spine surgeries are performed under general anesthesia. In select cases, regional anesthesia or spinal blocks may be used, allowing patients to remain awake without sensation in the operative area.
Recovery After Minimally Invasive Spine Surgery
Minimally invasive techniques can shorten hospital stays, with some patients returning home the same day. While discomfort is expected, muscle preservation often results in less postoperative pain compared to open surgery.
Physical therapy may be recommended depending on the procedure and overall health of the patient. Walking is typically encouraged early. If a fusion is performed, bone healing may take several months, and a brace may be recommended to maintain alignment during recovery.
Return to normal activities varies depending on the procedure performed and individual healing progress.
Risks Of Minimally Invasive Spine Surgery
Although minimally invasive surgery reduces tissue disruption, it carries risks similar to open surgery. Potential complications may include:
- Infection – Antibiotics are regularly given to the patient before, during, and often after surgery to lessen the risk of infections.
- Bleeding – A certain amount of bleeding is expected, but this is not typically significant.
- Pain at bone graft site – If your surgeon chooses to obtain bone from your hip or other areas you may experience persistent pain at the bone graft site.
- Recurrence of symptoms – Some patients may experience a recurrence of their original symptoms.
- Pseudarthrosis (failed fusion) – Patients who smoke, have diabetes, and/or renal failure are more likely to develop a pseudarthrosis or failed fusion. This is a condition where there is not enough bone formation. If this occurs, a second surgery may be required in order to obtain a solid fusion.
- Nerve or blood vessel injury – It is possible that the nerves or blood vessels may be injured during these operations. These complications are very rare.
- Blood clots – Another uncommon complication is the formation of blood clots in the legs. These pose significant danger if they break off and travel to the lungs. Blood clots often occur due to prolonged periods of immobility which is unusual with MIS surgery.
Modern techniques and careful surgical planning help minimize these risks.
Why Choose Princeton Neurological Surgery For Minimally Invasive Spine Surgery?
Minimally invasive spine surgery requires technical expertise, precise imaging guidance, and careful patient selection. Princeton Neurological Surgery is led by board-certified neurosurgeon Dr. Edward H. Scheid, Jr., who has performed more than 6,000 spine surgeries and is experienced in both open and minimally invasive techniques. Our team evaluates each case individually to determine whether minimally invasive surgery is appropriate or whether traditional open surgery would provide safer or more effective results. Patients in Hamilton and Jersey City trust our practice for advanced spine care that prioritizes safety, precision, and long-term outcomes.
Minimally Invasive Spine Surgery Consultation In Hamilton, NJ
If you are exploring options for spine surgery, Princeton Neurological Surgery in Hamilton, NJ serves patients from Hamilton and Jersey City—call (609) 890-3400 to schedule your consultation and learn whether minimally invasive spine surgery may be right for you.