The spine is made up of a series of bones called vertebraee stacked one on top of another. Between each vertebrae sits an intervertebrael disc that acts as a cushion and shock absorber. These discs are round and relatively flat, with a durable outer layer and a soft, gel-like center. Their structure allows the spine to bend, twist, and move while maintaining space for nearby nerves to exit the spinal canal. Because of their position and constant use, spinal discs are vulnerable to wear, degeneration, and injury.
At Princeton Neurological Surgery, patients in Hamilton, NJ and Jersey City receive comprehensive evaluation and treatment for herniated discs and other spinal conditions. The practice is guided by the leadership of Dr. Edward H. Scheid, Jr., a board-certified neurosurgeon who has performed more than 6,000 successful spine surgeries. With a careful, step-by-step diagnostic approach, the team works to identify the precise cause of pain and develop a treatment plan tailored to each individual.
What Is A Herniated Disc?
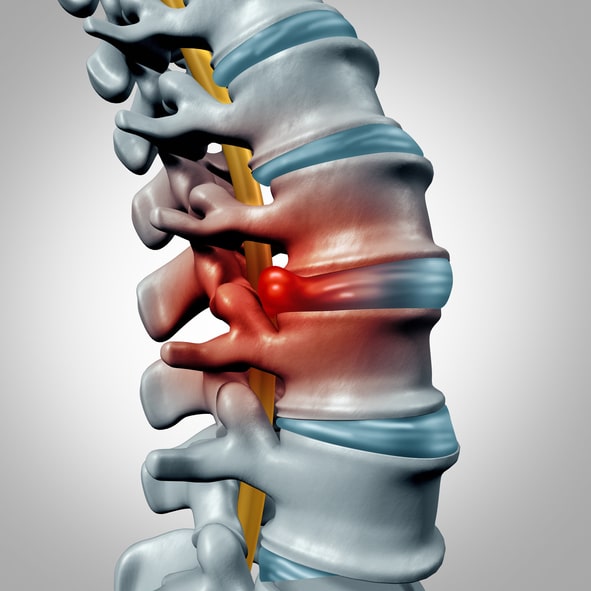
A herniated disc occurs when the outer fibrous layer of an intervertebrael disc tears or cracks, allowing some of the inner gel-like material to bulge or break through. This condition most commonly affects the lumbar spine, or lower back, and is a frequent cause of back pain. Herniated discs can also occur in the cervical spine, leading to neck and shoulder pain.
When a disc becomes damaged, it may:
- Protrude outward and press on nearby nerve roots
- Leak inner material that irritates surrounding nerves
- Narrow the space where nerves travel
If the herniated disc does not contact a nerve, a person may experience little to no pain. However, when nerve compression or inflammation occurs, symptoms can become significant.
Herniated Disc Symptoms
Symptoms depend on the location of the affected disc and whether a nerve is involved.
Common symptoms include:
- Back or neck pain
- Numbness or tingling in an arm or leg
- Muscle weakness
- Pain radiating into the buttock and down the leg, known as sciatica
Pain may worsen with activities that increase pressure on the spine, such as coughing, sneezing, sitting, or bending forward. Some individuals notice improvement with rest.
In certain cases, progressive nerve compression can lead to more serious neurological changes, including loss of sensation or reduced muscle control.
What Causes A Herniated Disc?
A disc may become herniated when persistent or extreme pressure is placed on it by the surrounding vertebraee. This pressure can force the inner gel-like material through a weakened area of the outer shell.
Most herniated discs develop gradually due to age-related degeneration. As discs lose hydration and elasticity over time, they become more susceptible to tearing.
Risk factors include:
- Natural disc degeneration due to aging
- Excess body weight
- Traumatic injury, such as a fall or car accident
- Lifting heavy objects with improper technique
While lumbar herniations are the most common, discs in the neck and mid-back may also be affected
Herniated Disc Vs. Bulging Disc
The terms “slipped disc” and “herniated disc” are often used interchangeably. A bulging disc, however, is slightly different.
With a bulging disc, the outer fibrous layer remains intact, but the disc extends outward around part or all of its perimeter due to structural changes. A herniated disc involves a tear in the outer annulus, allowing the inner material to protrude outward. Because the inner substance can irritate or compress nerves, herniated discs are more likely to cause pain.
Diagnosing A Herniated Disc
Diagnosis begins with a detailed medical history and physical examination. Your provider will assess posture, reflexes, muscle strength, and sensation to evaluate nerve involvement.
Imaging studies are often used to confirm the diagnosis, including:
- MRI scans to visualize discs and nerves
- Additional imaging when needed to clarify findings
A thorough evaluation helps rule out other conditions and guides treatment planning.
Treatment Options For A Herniated Disc
Treatment depends on symptom severity, disc location, and nerve involvement. Many herniated discs improve over time with conservative management.
Non-surgical treatment may include:
- Rest and activity modification
- Heat therapy
- Physical therapy and therapeutic exercises
- Prescription pain medication
- Posture correction strategies
Surgery is generally considered when conservative therapies do not provide lasting relief or when neurological deficits worsen.
Surgical Treatment For Herniated Disc
When surgery is necessary, several techniques may be considered based on the clinical situation:
- Discectomy to remove the damaged portion of the disc
- Laminotomy to relieve pressure on a nerve root
- Arthroplasty to replace part or all of the disc
- Spinal fusion to stabilize the spine when appropriate
The goal of surgical treatment is to relieve nerve compression and achieve meaningful, lasting pain relief while maintaining spinal stability.
When Is Surgery Required For A Herniated Disc?
Surgery is typically considered when conservative treatments fail to provide adequate relief or when neurological symptoms worsen.
Surgical intervention may be recommended if:
- Pain persists despite months of non-surgical care
- Progressive muscle weakness develops
- Significant nerve compression is confirmed on imaging
- Loss of sensation or motor control occurs
In rare cases involving traumatic injury or severe neurological compromise, surgery may be recommended more urgently.
The decision to proceed with spinal surgery is made carefully after reviewing clinical findings, imaging results, and the patient’s overall health and functional limitations. The primary objective is to achieve lasting pain relief and prevent permanent nerve damage.
Why Choose Princeton Neurological Surgery For Herniated Disc Treatment?
Princeton Neurological Surgery is guided by the expertise of Dr. Edward H. Scheid, Jr., a board-certified neurosurgeon and President and Founder of NeuroSpine Plus, LLC. With more than 6,000 spine surgeries performed, the practice offers extensive experience in treating disc herniation, spinal stenosis, cervical myelopathy, degenerative disc disease, and other complex spinal conditions.
What distinguishes the team is its individualized, methodical approach. Each patient undergoes a careful evaluation to determine the exact source of pain before a customized treatment plan is developed. The practice utilizes advanced techniques, including minimally invasive procedures when appropriate, with a focus on preserving neurologic function and improving quality of life. Patients in Hamilton and Jersey City benefit from experienced, patient-centered spine care delivered close to home.
Herniated Disc Treatment In Hamilton, NJ
A herniated disc can range from mildly uncomfortable to severely limiting. While some cases improve with conservative care, others require surgical intervention to relieve nerve compression and prevent worsening symptoms.
Princeton Neurological Surgery provides advanced spine care in Hamilton, NJ and serves patients from Jersey City and surrounding communities. To schedule a consultation, call Princeton Neurological Surgery in Hamilton, NJ at (609) 890-3400 today.