Revision spinal surgery is performed when a patient continues to experience persistent, recurrent, or new symptoms after a prior spine procedure. In many cases, pain improves within several months of the initial surgery. However, when symptoms such as chronic pain, instability, weakness, or neurologic dysfunction remain unresolved, a second operation may be necessary to address the underlying cause.
At Princeton Neurological Surgery, revision procedures are performed by a neurosurgical team led by board-certified neurosurgeon Dr. Edward H. Scheid, Jr., who has performed more than 6,000 spine surgeries. Revision surgery requires precise diagnosis and advanced technical expertise, particularly when addressing failed cervical disc replacement, pseudarthrosis after fusion, hardware complications, or persistent nerve compression. Patients in Hamilton and Jersey City, NJ trust our team to carefully evaluate prior procedures and develop a thoughtful corrective surgical plan.
Why Revision Spine Surgery May Be Necessary
Revision surgery is most commonly performed in the cervical or lumbar spine. Causes may include:
- Failed fusion (pseudarthrosis)
- Re-herniated disc
- Recurrent or worsening spinal stenosis
- Hardware loosening or breakage
- Infection
- Adjacent segment degeneration
- Spinal instability
- Incomplete decompression from the initial surgery
In some cases, degeneration progresses naturally over time at levels adjacent to the original surgical site. In others, structural healing does not occur as expected, leading to instability or ongoing nerve compression.
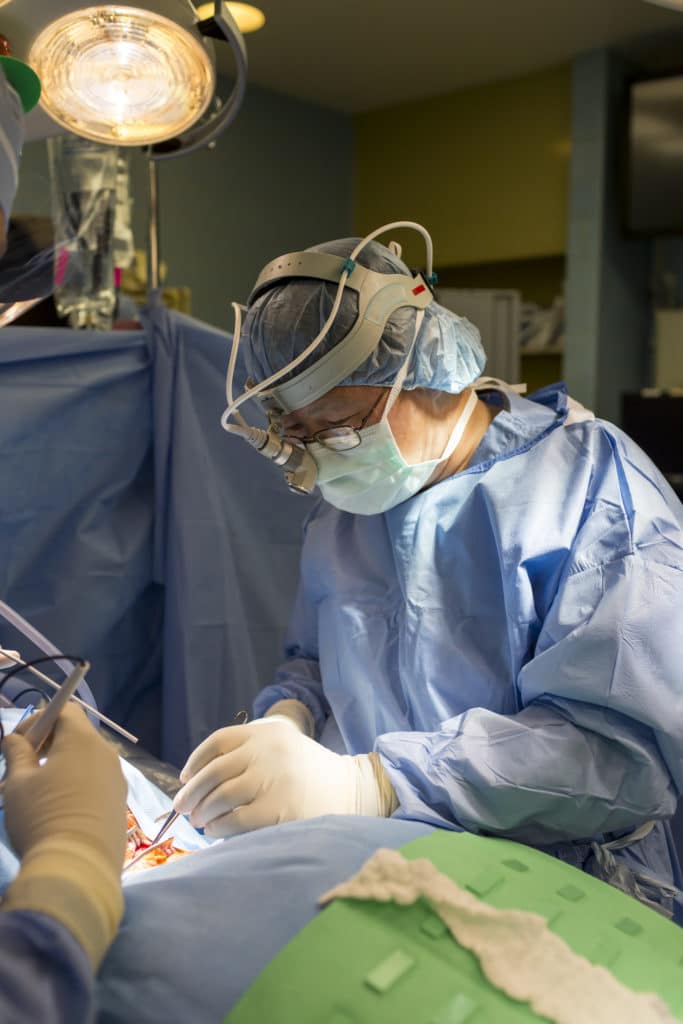
When Ongoing Symptoms Suggest A Second Evaluation
Most patients expect steady improvement after spine surgery. When recovery stalls, symptoms return, or new neurologic issues develop, a careful reassessment is necessary.
Revision surgery may be considered when pain never fully resolved, returns after a period of improvement, or changes in character. For example, a patient who previously had leg pain relieved by surgery may begin experiencing new shooting pain, progressive numbness, or muscle weakness. In other cases, symptoms may suggest spinal instability, hardware complications, or incomplete decompression of a nerve.
More urgent evaluation is required if bowel or bladder dysfunction develops or if neurologic deficits worsen. These symptoms warrant prompt imaging and specialist review to determine whether structural issues remain unaddressed.
Common Causes Of Failed Spine Surgery
Spine surgery is highly nuanced, and failure does not necessarily indicate negligence or error. Healing outcomes vary based on biological and mechanical factors.
Common contributors to failed spine surgery include:
- Failure of two vertebraee to successfully fuse
- Scar tissue formation around a nerve root
- Inadequate decompression
- Recurrent disc herniation
- Adjacent segment disease
- Secondary pain generators not addressed in the original operation
Because revision surgery must address both the original pathology and any new structural changes, thorough reassessment is critical.
How Revision Spinal Surgery Is Performed
The surgical approach depends entirely on the identified cause of failure. When fusion has not occurred, revision may involve removing or replacing hardware, placing new bone graft material, and potentially using bone growth stimulation techniques.
If nerve compression persists, further decompression may be required to remove bone, ligament, or disc material. In cases of hardware failure or instability, instrumentation may be revised or reinforced.
Scar tissue and altered anatomy often make revision procedures more technically demanding than first-time surgeries, requiring careful surgical planning and precision.
Recovery After Revision Spine Surgery
Most revision spine procedures require a hospital stay of several days. Early walking is encouraged to promote circulation and reduce the risk of blood clots. Activity restrictions commonly include avoiding bending, lifting, and twisting during early healing.
Initial recovery typically ranges from six weeks to three months, depending on the complexity of the procedure. If spinal fusion is involved, bone healing continues over several additional months. Physical therapy may be recommended to restore strength and mobility.
Risks Of Revision Spine Surgery
Because revision surgery addresses prior structural changes and scar tissue, it carries higher risks than primary spine surgery. Potential complications include:
- Infection
- Delayed wound healing
- Nerve injury
- Blood clots
- Hardware complications
- Failure to achieve solid fusion
Careful surgical planning and post-operative compliance help reduce these risks.
Frequently Asked Questions About Revision Spinal Surgery
Why Choose Princeton Neurological Surgery For Revision Spine Surgery?
Revision spine surgery requires advanced diagnostic evaluation and significant surgical experience. Princeton Neurological Surgery is led by board-certified neurosurgeon Dr. Edward H. Scheid, Jr., who has performed more than 6,000 spine surgeries and has extensive experience correcting failed cervical and lumbar procedures. Our team carefully reviews prior imaging, operative reports, and current symptoms to identify the precise source of ongoing pain or instability. We develop individualized surgical strategies focused on restoring stability, relieving nerve compression, and improving neurologic function. Patients in Hamilton and Jersey City rely on our expertise when previous spine surgery has not delivered the relief they expected.
Revision Spine Surgery Consultation In Hamilton, NJ
If you continue to experience persistent pain or neurologic symptoms after prior spine surgery, Princeton Neurological Surgery in Hamilton, NJ serves patients from Hamilton and Jersey City—call (609) 890-3400 to schedule your consultation and determine whether revision spinal surgery may be appropriate for you.