The choice to undergo radiosurgery is a decision that requires careful research. Most patients have similar questions when beginning to learn about radiosurgery and radiosurgery treatments.
What is Radiosurgery?
Stereotactic Radiosurgery (SRS) is a non-invasive medical procedure designed to treat benign and malignant lesions within the body. SRS uses the principles of stereotaxy, or 3-D target localization, with multiple cross-fired beams from a high-energy radiation source to precisely irradiate the target. While a single beam of radiation is innocuous to the surrounding tissue, the culmination of cross-fired beams at the target is destructive. This technique allows for the delivery of aggressive dosing to the target, while protecting surrounding healthy tissue. Stereotactic Radiosurgery is also known as stereotactic radiotherapy (SRT) when used to target lesions in the brain, and stereotactic body radiotherapy (SBRT) when used to target lesions in the body. In addition to cancer, it has also been shown to be beneficial for the treatment of some non-cancerous conditions, including vascular disorders such as arteriovenous malformations (AVMs) and chronic pain disorders such as trigeminal neuralgia. Radiosurgery is used to destroy target tissue that is otherwise inaccessible or too risky for open surgery. In some cases, it can be used as an alternative treatment option for those who are unwilling or unable to undergo an open surgical procedure. There are many conditions for which conventional surgical treatment is difficult or inadvisable due to potential deleterious consequences for the patient, such as damage to nearby vascular structures, nerves, and other vital structures. Radiosurgery has thus been especially helpful for the localized, highly precise treatment of brain and spine tumors.
What is Radiosurgery used to treat?
Radiosurgery is indicated primarily for the treatment of tumors, vascular lesions, and functional disorders. Significant clinical judgment must be used with this technique and considerations must include tumor type, size, location, and knowledge of surrounding critical structures including their function and dose tolerance. General contraindications to radiosurgery include excessively large size (> ~3-4cm) target lesions or lesions too numerous for practical treatment.
Patient Outcome
Outcome from radiosurgery is usually delayed because its biological effects on the target tissue may take months after treatment delivery. Different tissues or cell types may be more or less sensitive to radiation and this will determine when a specific cell type will be affected after treatment. For example, a patient’s back pain created by a spinal tumor may improve within hours or days after treatment because the pain mediating inflammatory cells incited by the tumor are likely more sensitive to radiation than the tumor itself. Destruction of tumor cells on the other hand may take several weeks or months. Since radiosurgery does not remove the tumor, but results in a biological inactivation of the tumor, lack of growth of the lesion is normally considered to be treatment success. Lack of tumor growth generally results in the prevention of surrounding inflammation, pain, and destruction of surrounding critical structures.
Treatment Process
Typically, radiosurgery is administered in 1-5 daily fractions over consecutive days. Nearly all radiosurgery treatments are given on an outpatient basis without the need for anesthesia. Treatment is usually well tolerated with few if any side effects, requires no recovery time, and only very rarely interferes with a patient’s quality of life. To see what tools we use at the Brain and Spine Radiosurgery Institute, visit our Radiosurgery Treatment Tools page here.
What is the difference between Radiation Therapy (RT), Intensity Modulated Radiation Therapy (IMRT) and Radiosurgery?
Traditional radiation therapy (RT) typically delivers radiation to a wide field of tissue in the body resulting in the treatment of both the tumor and a large amount of surrounding healthy tissue. This technology is ideal for tumors that invade the surrounding tissue and when tumor margins are not well defined. Intensity modulated radiation therapy or IMRT is similar to traditional radiation therapy with the exception that intensity modulation is used to curve dose delivery more closely along tumor margins compared to RT. These relatively wide radiation fields increase the possibility of damage to normal tissue which increases the risk of side effects following radiation treatment. In an effort to protect healthy tissue, traditional RT and IMRT are delivered in small daily doses or fractions divided into 30-40 treatment sessions. This dosing strategy is commonly referred to as hyperfractionation. The sub-lethal daily doses allow healthy tissue to repair itself; a capability not present in tumor cells. However, the final dose delivered to the patient is limited by the tolerance of healthy tissue in close proximity to the target. This limitation may result in the inability to adequately control tumor growth. Regardless, once a patient has received his or her limit, radiation treatment must stop in an effort to prevent healthy tissue damage.
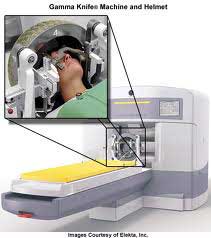
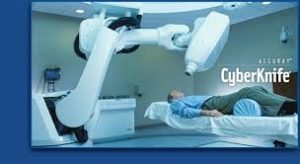
Radiosurgery devices, such as the Gamma Knife and CyberKnife were designed to deliver high dose radiation with extreme accuracy, targeting the tumor with minimal damage to the surrounding healthy tissue. This enables higher more effective dosing to stubborn tumor cells using extreme precision to protect healthy tissue as opposed to hyperfractionation. Traditionally, radiosurgery was delivered in a single session or fraction. The ablation of the target tissue within a single fraction was compared to the definitive cut using a surgeon’s scalpel; hence the term radiosurgery. However, even with extreme precision, in some cases such as with tumors located within the brain or spinal cord, hypofractionation (i.e., 2-5 fractions) becomes necessary when protection of even a very small amount of healthy tissue is critical. The CyberKnife System was one of the first radiosurgery devices to use hypofractionation as an added measure of safety. This allows for less damage to surrounding healthy tissue and for clinicians to complete treatment in 1 to 5 days compared to several weeks required for traditional RT or IMRT.
What are the differences between the various Radiosurgery treatment tools?
History of Radiosurgery Tools
The first major radiosurgery device was introduced by Swedish neurosurgeon Dr. Lars Leksell with the invention of the Gamma Knife in 1968. At the time, Dr. Leksell considered three separate sources of radiation including radioactive cobalt (gamma rays), linear accelerator (LINAC) (high-energy x-rays) and positively charged particles (proton beam). For practical and technical reasons, Dr. Leksell chose cobalt-60 as the radiation source for Gamma Knife. The targeting strategy of Gamma Knife is based on the fact that the location of any target is fixed relative to points of reference on the skull. A rigid head frame fixed to the skull that employs three dimensional stereotactic coordinates can therefore be used for precise targeting of a brain tumor. The traditional head frame limits the use of Gamma Knife to treatment of intracranial targets and therefore does not allow for spinal or body radiosurgery. The Gamma Knife was later introduced in the United States in 1987 by Leksell protégé, Dr. L. Dade Lunsford, a neurosurgeon at the University of Pittsburgh Medical Center. The Gamma Knife has since been used successfully and reliably for treatment of targets confined within the skull.
With advances in technology, in 1994 Stanford neurosurgeon Dr. John Adler introduced the CyberKnife which uses a LINAC as the radiation source mounted on a robotic arm. Having also been a student under Dr. Leksell, Dr. Adler sought to create a radiosurgery device that can be used in other areas of the body in a more comfortable manner without a rigid head frame. It was also believed that the nearly limitless degrees of freedom of the robotic arm allowed for more versatile dose coverage of irregularly shaped targets. Other LINAC radiosurgery technology evolved as well such as the Varian TrueBeam STx™ (produced by Varian and BrainLab) and Elekta Synergy® S. A major difference between these technologies and CyberKnife is that the LINAC in the former is housed within a gantry arc rather than being attached to the head of a rotating robotic arm as in CyberKnife.
Radiosurgery Tools Today
As manufacturers of radiosurgery devices compete with one another, technical differences are often highlighted in an attempt to claim superiority. The major differences involve the source of radiation and the way in which the device tracks a target within the body. Each manufacturer has developed a unique strategy to achieve precision targeting. The Gamma Knife and LINAC gantry arc-based systems commit multiple radiation beams to a target that is positioned at the center of the radiation field. Once the target is fixed in position, any movement during treatment would result in an inaccurate delivery of radiation. Therefore, Gamma Knife and some LINAC arc-based systems employ the use of a rigid head frame for intracranial targeting where submillimeter accuracy is required. CyberKnife, on the other hand, delivers single radiation beams in succession to a target that is localized in three dimensional space. During treatment, x-rays are used to track and correct for patient movement which allows the Cyberknife robotic arm to follow the target throughout treatment delivery. Furthermore, without the need for rigid fixation, CyberKnife allows for hypofractionation (i.e. delivery of radiation over 2-5 consecutive days) that is further used to protect healthy tissue. To compete with advanced frameless technology and to allow for hypofractionated treatment, Novalis Tx (BrainLab) and Trilogy (Varian) also developed non-invasive immobilization devices coupled with real-time imaging to detect patient motion during treatment. Gamma Knife (Elekta) recently introduced Extend™ system, a non-invasive mouthpiece used for cranial stabilization purposes. However, similar to frameless intracranial options used by some LINAC gantry arc-based systems, the Extend™ option is often substituted by a traditional rigid head frame when extreme accuracy is required.
With respect to different radiation sources, both gamma rays (Gamma Knife) and high-energy X-rays (LINAC) produce photon energy that has similar effects (Compton-scatter) on target tissue. Proton energy on the other hand has different properties (Bragg-peak) compared to photons with respect to how energy is released within a tissue. Often the physical properties of protons VS photons become the focus of advertising campaigns as opposed to their practical use in the clinical setting. It is important for your doctor to understand and recognize the select cases in which protons VS photons may become clinically significant.
Different radiosurgery technologies often require different treatment planning strategies. Furthermore, intracranial VS extracranial radiosurgery (e.g., spinal radiosurgery) require distinct levels of skill and training. In experienced hands, the differences among radiosurgery technologies should not change the clinical outcome. A skilled radiosurgeon is expected to create a treatment plan that is both safe and effective. Determining dose allocation to the target and setting limits to critical structures as well as determining the appropriate fractionation schedule are all factors that ultimately have the greatest effect on outcome. However, in select cases, the differences among these technologies may be important. It is therefore necessary that your neurosurgeon recognize these situations in order to make the appropriate treatment plan.
Gamma Knife VS CyberKnife
Gamma Knife VS CyberKnife
The first major radiosurgery device was introduced by Swedish neurosurgeon Dr. Lars Leksell with the invention of the Gamma Knife in 1968. Gamma Knife uses radioactive cobalt as the radiation source. The targeting strategy of Gamma Knife is based on the fact that the location of any target is fixed relative to points of reference on the skull. A rigid head frame fixed to the skull that employs three dimensional stereotactic coordinates can therefore be used for precise targeting of a brain tumor. The head frame limits the use of Gamma Knife to treatment of intracranial targets and therefore does not allow for spinal or body radiosurgery.
With advances in technology, in 1994 Stanford neurosurgeon Dr. John Adler introduced the CyberKnife which uses a LINAC (a machine that produces high energy x-rays) as the radiation source mounted on a robotic arm. Having been a student under Dr. Leksell, Dr. Adler sought to create a radiosurgery device that can be used in other areas of the body in a more comfortable manner without a rigid head frame. It was also believed that the nearly limitless degrees of freedom of the robotic arm allowed for more versatile dose coverage of irregularly shaped targets.
The major differences between Gamma Knife and CyberKnife involve the source of radiation and how radiation is delivered to the target. With respect to the radiation sources, both gamma rays (Gamma Knife) and high-energy X-rays (CyberKnife) produce photon energy that has similar effects (Compton-scatter) on target tissues.
The targeting methods are perhaps the major differences between the two technologies. The Gamma Knife is frame based, which means it requires a rigid head frame that is fixed to the patient’s skull during treatment while the CyberKnife is frameless. The Gamma Knife commits multiple radiation beams to a target that is positioned at the center of the radiation field. Once the target is fixed in position, multiple small cylindrical collimators open to expose the target to radiation in a controlled manner. Any movement of the target during treatment would result in an inaccurate delivery of radiation. Hence the reason why Gamma Knife employs a rigid head frame for intracranial targeting.
CyberKnife, on the other hand, delivers single radiation beams in succession to a target that is localized in three dimensional space. During treatment, x-ray guidance is used to track and correct for target movement which allows the CyberKnife robotic arm to follow a target throughout treatment delivery. Furthermore, without the requirement for rigid fixation, CyberKnife allows for hypofractionation (i.e. delivery of radiation over 2-5 consecutive days) a technique that is used to protect healthy tissue, especially when targets are embedded within critical structures such as the spinal cord or brain stem.
A common question often arises as to which device is most accurate. The answer is a bit complicated since the two targeting strategies are very different. Both technologies deliver radiation to an accuracy of less than 1 millimeter. However most will argue that the frame-based system (Gamma Knife) is slightly more accurate compared to the frameless system (CyberKnife). However, although accuracy is important, the ultimate effect on the target tissue also depends upon how dose is distributed to the target. For example, Gamma Knife uses isocentric targeting whereas CyberKnife uses non-isocentric targeting. This basically refers to the way radiation dose is distributed to a target (Gamma knife uses overlapping spheres or isocenters whereas CyberKnife uses more conformal dose coverage). Lastly, CyberKnife often employs hypofractionation that further distinguishes the two technologies and their respective targeting strategies.
Since Gamma Knife and CyberKnife are different technologies, they require different treatment planning strategies. In experienced hands, the differences among these two radiosurgery technologies should not change the clinical outcome. A skilled radiosurgeon is expected to create a treatment plan that is both safe and effective. Determining dose allocation to the target and setting limits to critical structures as well as determining the appropriate dosing schedule are all factors that ultimately have the greatest effect on outcome. However, in select cases, the differences among these two technologies may be important. It is therefore necessary that your neurosurgeon recognize these situations in order to design the best treatment plan.
What are the potential risks and side effects of Radiosurgery?
The outcome of radiosurgery procedures is generally good in skilled and experienced hands. However, understanding the risks and benefits is essential to making a sound and informed decision with your doctor and family prior to undergoing treatment. One of the most concerning risks of radiosurgery is failure to control continued growth of a tumor or to be ineffective at achieving the desired outcome. If a brain or spinal tumor continues to enlarge, it may invade or compress surrounding critical neural structures that control mental, motor, or sensory functions. In most cases however, further tumor growth is gradual and alternative intervention can often be pursued to help prevent worsening symptoms. Your neurosurgeon can give you a more detailed explanation regarding the likely side effects of continued tumor growth based on its particular anatomical location.
Another possible side effect of radiosurgery is damage to critical neural structures from radiation exposure. Although radiosurgery can be directed to a target within a millimeter of accuracy, a limited amount of exposure to nearby critical structures is unavoidable. This point is most critical when dealing with brain and spine tissue that is often unforgiving if injured. A well-trained and experienced radiosurgeon must determine how much radiation is required to control tumor growth and how much exposure to critical structures is tolerable in order prevent serious side effects. Traditionally, this decision is a team approach that involves both a neurosurgeon and radiation oncologist. Understanding the balance between too much and too little radiation exposure is crucial to achieving the desired outcome.
Other rare potential side effects of radiosurgery depend largely on tumor anatomical location and may include transient generalized fatigue, nausea, headaches, seizures, sensory or motor changes, and in extremely rare cases, paralysis. It is important to discuss potential risks and benefits of treatment, alternative treatment options, and risks of no treatment with your doctor.
Does Radiosurgery cause nausea and vomiting?
Nausea and vomiting are extremely rare acute side effects that can occur within 12 hours of radiosurgical treatment. As radiosurgery delivers high dose radiation to intracranial tumors (brain tumors), it can cause swelling of brain tissue around the treated area. Nausea and vomiting usually occurs when lesions treated are within or near the brainstem and fourth ventricle where the vomiting center is located (area postrema). Swelling in this area may induce nausea and vomiting (depending on dose of radiation). Treatments include the prescription of steroids to reduce brain swelling and hence the nausea and vomiting and/or anti-emetics (anti-nausea medication). As with every medical procedure, not every patient will react in the same way to treatment.
Fortunately, we have not had this problem with any of our patients at Brain and Spine Radiosurgery Institute to date. We have an extremely high patient satisfaction rate. You can learn more by reading our Patient Testimonials.
Will Radiosurgery cause me to lose my hair?
Hair-loss from radiosurgery can occur, especially when the lesion treated is located just below the skin surface. The hair loss is caused by the radiation beam that affect the hair follicles. Usually with radiosurgery there is only a small patch of hair that is temporarily affected about the size of a golf ball or smaller. Regrowth of your hair is dependent on the dose of radiation administered. If you are concerned about hair loss due to radiosurgery, be sure to talk to your doctor pre-treatment.
Can radiosurgery cause damage to my sense of sight, smell, touch, taste and hearing?
Radiosurgery is an advanced and precise method of delivering radiation to intracranial (brain) cancer cells. Actually, one of the main benefits of radiosurgery is that it’s possible to deliver effective radiation, with fewer side effects than traditional radiotherapy treatment. Radiosurgery can deliver high doses of radiation with surgical precision, which decreases the likely hood of surrounding, healthy brain tissue, being affected. Although no medical treatment is without risk, the chance of radiosurgery damaging one of your 5 senses is unlikely. The risk depends on the proximity of the treated lesion to the cranial nerve or brain region that controls your senses. Every effort is made to protect and preserve your normal function while effectively treating your tumor.
What type of brain and spinal conditions can be treated using Radiosurgery?
Radiosurgery can often be used effectively to treat both benign and malignant brain and spinal tumors. Benign or non-cancerous tumors that can be treated using radiosurgery include meningiomas, schwannomas, pituitary adenomas, acoustic neuromas, neurofibromas, glomus tumors and others. Primary malignant tumors that may be treated either initially or for disease recurrence may include astrocyomas, oligodendrogliomas, pineal region tumors, and chordomas. Metastatic disease to the brain or spine including lung, prostate, breast, colon, rectal, melanoma, nasopharyngeal and others can also be effectively treated using radiosurgery. Other conditions treated using radiosurgery include trigeminal neuralgia, and arteriovenous malformations (AVMs).
Ideally, radiosurgery is reserved for tumors less than or equal to 3-4cm in diameter. Larger tumors that compress vital structures in the brain or spine may require surgical evacuation and therefore are not suitable for treatment using radiosurgery. Likewise, spinal tumors that invade the vertebral column and cause spinal instability also require surgical intervention. Therefore, it is best for tumors to be discovered early before they produce significant tissue damage to be ideal for radiosurgery. After treatment, it is important to follow a patient both clinically and radiographically in order to assess the treated lesion and to rule out evidence of new disease. Treatment of metastatic disease is often multifactorial and involves both chemotherapy and some form of radiation. Ultimately, the final decision regarding whether radiosurgery is an appropriate option for you will be made after a detailed evaluation and thorough discussion with your doctor.
What are some options for treating Brain and Spine Cancer?
Radiosurgery
Radiosurgery, also known as stereotactic radiosurgery, is a form of radiation and despite its name is not surgery. It is designed to precisely destroy a tumor or lesion by delivering a very high dose of radiation to the tumor in 1 to 5 treatments over a treatment course of 1 to 5 days. Patients are not required to be hospitalized during treatment and the procedure, using one of our radiosurgery tools, is almost always performed on an outpatient basis.
Radiation Therapy
Radiation therapy is a form of radiation that is usually delivered 5 days a week over a treatment course of 6 to 8 weeks. Radiation therapy, (as opposed to stereotactic radiosurgery), usually treats larger areas that include not only the tumor, but large amounts of healthy tissue (e.g., brain and spinal cord), increasing the risk of possible complications. Patients are not required to be hospitalized during treatment and the procedure is almost always performed on an outpatient basis.
Surgery
Surgery or surgical resection is an invasive procedure that requires an incision to remove or cut the tumor out of the body. Surgery can be performed on an inpatient or outpatient basis depending on the tumor being treated. Because of the invasiveness of some types of surgery, some patients may be excluded from receiving this type of treatment.
Radiosurgery Treatment FAQ’s
How long will it take for radiosurgery to reduce the back pain caused by my spinal tumor?
A spinal tumor causes back pain due to its involvement within the bones that make up the spinal column. Sometimes the bones can weaken and collapse due to tumor involvement which can cause extreme pain and neurologic deficits such as sensory loss, weakness, and paralysis. Radiosurgery does not remove the tumor; it makes the tumor biologically inactive. The radiation acts on the DNA within the tumor cells that ultimately leads to tumor death. This process can take several weeks to months. The good news is that the pain reduction process works much faster. The radiation does not just affect the cancer cells but also the pain mediating inflammatory cells. An improvement in back pain can be felt as soon as hours after treatment. As the growth of the tumor is halted over the coming weeks and months, a further relief of pain will be felt. Once the tumor has been successfully treated, bony integrity is eventually restored.
Will I be radioactive after my radiosurgery treatment; are there any precautions I should take?
No, you will not be radioactive after radiosurgery treatment. The radiation causes the cancerous cells to die, by creating injury to their DNA. The treatment does not make the cells radioactive, nor the patient.
Will I experience pain during my radiosurgery?
Radiosurgery is a painless treatment. Not only is it pain free, but the patient is awake for the whole process. You can communicate with the treatment team during the radiosurgery procedure and even request rest room breaks. You can bring your favorite music and we will play it for you during your treatment.
I am a patient with an extensive medical history, am I considered safe for radiosurgery treatment?
Radiosurgery is considered a valuable approach to treat cancer in higher risk patients. It is a safer and effective alternative to open brain surgery, as patients do not require anesthesia or a surgical incision. If you are extremely anxious prior to your treatment you can discuss this with your doctor and a mild sedative can be administered. There is no risk of hemorrhage, infection, increased hospital stay, or a long recovery period; as these risks are associated with open brain surgery.Also, radiosurgery gives patients who may have an inoperable tumor (due to location of tumor or health condition), the option of treatment.
Will I need to take time off work for treatment and the recovery period?
With radiosurgery, patients do not need to stay in the hospital, and their recovery time is minimal. There may be, depending on your condition, some restrictions the day you receive the radiosurgery treatment. It is expected that you proceed through your daily activities post treatment. Actually, sometimes Dr. Lipani and I treat patients on their lunch break. Our team will make every attempt to schedule your treatment at a time of day that works best for you. We treat our patient’s like family. Talk to your nurse and physician about any questions or concerns you may have. We want our patients to receive extra special care and attention they deserve.
If you would like more information about our services or to schedule an appointment, feel free to fill out our convenient contact form or call us directly at (609) 890-3400.